Cataract, Refractive, Refractive Surgery, Artificial Intelligence
Improving Preoperative Prediction of PCR
Machine learning models show promise, outperforming existing scoring systems.

Cheryl Guttman Krader
Published: Friday, March 1, 2024
“ Analysing data for PCR risk prediction is challenging because PCR is rare. “
Posterior capsule rupture (PCR) occurs in approximately 1% of cataract surgery cases and is a feared event because of its potential sight-threatening consequences.
Now, work is underway leveraging data reported to the European Registry of Quality Outcomes for Cataract and Refractive Surgery (EUREQUO) to see if a machine learning model could improve preoperative identification of patients at increased risk of PCR.1
Research conducted so far indicates such artificial intelligence-based classifiers outperform existing scoring systems and, therefore, if implemented in the clinic, may reduce the number of cases of PCR, said Rudy MMA Nuijts MD, PhD.
“Identification of patients at high risk for PCR is important so that these difficult cases can be assigned to experienced operators and for providing better communication to patients about their surgical risk,” said Dr Nuijts. “Existing scoring systems for PCR risk assessment are based on a subjective weighting of known risk factors. We were interested in seeing if data-driven risk assessment would estimate the probability of PCR more reliably and objectively.”
Three different probabilistic classifiers were constructed to estimate the probability of PCR before surgery. They included two discriminative models—a logistic regression model and a multi-layer perceptron network—and a generative model known as a Bayesian network, which has the advantage that it can deal with missing data, Dr Nuijts said.
“Analysing data for PCR risk prediction is challenging because PCR is rare, there is an exponential number of feature combinations, and, as in all registries, we have missing data.”
All the classifiers were trained using data from about 2.8 million cases of cataract surgery performed between January 2008 and December 2018. Performance of the classifiers was determined by calculating area under the precision-recall curve (AUPRC). The results showed the multi-layer perceptron network performed best followed by the Bayesian network and then the logistic regression model. The mean AUPRC for the three classifiers was 13.10, 8.05, and 7.31, respectively.
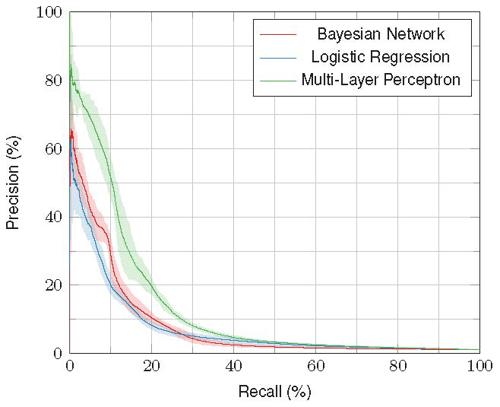
“The multi-layer perceptron performs better than subjective grading systems published in the literature,” Dr Nuijts said. “In addition, compared to a random classifier that has no knowledge of the patient or procedure, the machine learning classifiers are about 7 to more than 12 times better in generating the probability.”
Analysis of an independence graph generated by the Bayesian network model was also performed to characterise direct and indirect risk factors for PCR. Direct risk factors included preoperative best-corrected visual acuity, year of surgery, operation type, anaesthesia, target refraction, other ocular comorbidities, white cataract, and corneal opacities.
Going forward, further work aims to validate and compare the machine learning models using data from other registries, such as the American Academy of Ophthalmology’s Intelligent Research in Sight (IRIS) registry. Once the model is validated, Dr Nuijts envisioned the ideal situation as relevant information, including measurements from diagnostic systems, would automatically be entered into the electronic medical record, where they would be available to be processed in the probabilistic classifier.
“This would be the most efficient and beneficial way for surgeons to have an idea of the risk of PCR for any individual patient,” Dr Nuijts said.
Dr Nuijts spoke at the ESCRS Symposium during AAO Refractive Surgery Subspecialty Day 2023 in San Francisco, US. He acknowledged his co-authors—Dr Ron Triepels, Dr Maartje Segers, and Dr Mor Dickman.
1. Triepels RJMA, Segers MHM, Rosen P, et al. “Development of machine learning models to predict posterior capsule rupture based on the EUREQUO registry,” Acta Ophthalmol. 2023; 101(6): 644–650.
Rudy MMA Nuijts MD, PhD is Professor of Ophthalmology, Vice-Chairman, and Director of the Cornea Clinic and the Center for Refractive Surgery at the University Eye Clinic, Maastricht, Netherlands. rudy. nuijts@mumc.nl
Ron JMA Triepels PhD is assistant professor at the Department of Data Analytics and Digitalization of Maastricht University, Maastricht, Netherlands. r.triepels@maastrichtuniversity.nl
Maartje HM Segers MD is a PhD candidate at the University Eye Clinic, Maastricht University Medical Center+, Maastricht, Netherlands. maartje. segers@mumc.nl
Mor M Dickman MD, PhD is associate professor at the University Eye Clinic, Maastricht, Netherlands, and clinical co-director of the ESCRS registries. mor.dickman@mumc.nl
Latest Articles
Towards a Unified IOL Classification
The new IOL functional classification needs a strong and unified effort from surgeons, societies, and industry.
Organising for Success
Professional and personal goals drive practice ownership and operational choices.
Update on Astigmatism Analysis
Is Frugal Innovation Possible in Ophthalmology?
Improving access through financially and environmentally sustainable innovation.
iNovation Innovators Den Boosts Eye Care Pioneers
New ideas and industry, colleague, and funding contacts among the benefits.
José Güell: Trends in Cornea Treatment
Endothelial damage, cellular treatments, human tissue, and infections are key concerns on the horizon.
Making IOLs a More Personal Choice
Surgeons may prefer some IOLs for their patients, but what about for themselves?
Need to Know: Higher-Order Aberrations and Polynomials
This first instalment in a tutorial series will discuss more on the measurement and clinical implications of HOAs.
Never Go In Blind
Novel ophthalmic block simulator promises higher rates of confidence and competence in trainees.